Tonsillectomy Overview
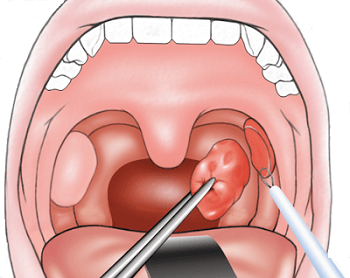 There are typically only a couple of reasons why your doctor would ever suggest tonsil removal, commonly known as a Tonsillectomy. Each year, over 500,000 Americans have their tonsils removed for one reason or another. One of these reasons may be due to chronic inflammation or infection of the tonsils. Those who experience frequent tonsillitis may consider a tonsillectomy as a way to remedy this issue.
There are typically only a couple of reasons why your doctor would ever suggest tonsil removal, commonly known as a Tonsillectomy. Each year, over 500,000 Americans have their tonsils removed for one reason or another. One of these reasons may be due to chronic inflammation or infection of the tonsils. Those who experience frequent tonsillitis may consider a tonsillectomy as a way to remedy this issue.
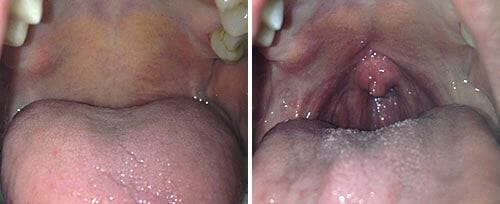
Another common reason why one may consider a tonsillectomy is if their physician has determined that their tonsils are oversized which can lead to issues with snoring or sleep apnea. Abnormally large tonsils can fall into the back of the throat and cause a partial or complete blockage of the airway. When a partial blockage occurs, the tonsils rattle around while breathing and generate the sound of snoring. In other cases, the tonsils completely block off the flow of air, causing an apneic episode which is when airflow stops momentarily, the body awakens and breathing resumes once again. Each episode can last for a few seconds to a minute or more. Most individuals with sleep apnea experience several apneic episodes each night.
Regardless of the reason, you may have been advised by your physician that a tonsillectomy is in your future. There are several techniques that are commonly used to remove tonsils, some more popular than others.
In the past, the dissection and snare technique was used in which forceps, scissors, and a snare are used to remove the tonsils. Today electrocautery (electrosurgery) is far more common and is a method that uses electrical energy to separate tonsil tissue from surrounding tissue. The device used to cut the tonsils generates concentrated energy that produces heat up to 800° F in order to cut through tissue. The energy and heat cause cells to rupture and tissue vaporizes. One of the greatest benefits of using this method is the fact that the heat cauterizes the tissue and bleeding is minimized.
There are several other methods that are used such as radiofrequency ablation, thermal welding, and the carbon dioxide laser.
One method that has gained popularity in recent years is Coblation, a method that was discovered by accident in the 1990’s.
Coblation Tonsillectomy
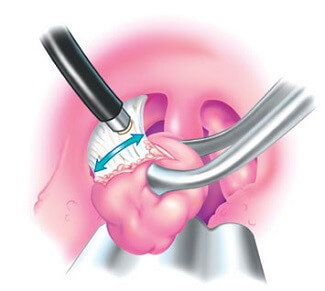
Coblation Tonsillectomy
A Coblation Tonsillectomy is a type of technology that was introduced by Hira V. Thapliyal and Philip E. Eggers in the mid 1990’s. They were in search of a method to unblock coronary arteries by use of electrosurgical energy. After realizing that their coblation wand could be used during surgeries such as tonsillectomies, they formed ArothoCare and began to market their product at the arthroscopy show in 1996.
The name Coblation can be broken down – Co, meaning controlled and blation which is derived from the word ablation, which means to reduce the size of something. A Coblation wand combines the use of a saline solution and radiofrequency to generate a plasma field.
What makes Coblation so unique is the fact that it generates very little heat. Unlike electrosurgery which generates heat upwards to 800° F, cobalation only reached around 175° F which is no hotter than a cup of coffee or tea. As a result, the healthy tissue in which the tonsils are cut from does not sustain the heat damage that typically occurs with electrosurgery.
A Closer Look at a Coblation System
Taking a closer look, the coblation system consists of four parts – The RF generator, foot pedal, irrigation system and wand.
The RF generator creates radiofrequency signals that can be used for either coblation or cauterization, depending on which setting is used. The foot pedals allow the surgeon to choose between each mode.
The wand is the tool that’s used to perform the procedure. Wands can be switched out and are available in several different sizes depending upon the application. The wand contains both active and passive electrodes which interact with the flow of a saline solution which turns into ions and forms plasma. It’s the plasma that cuts through the tissue.
Is Coblation Really Better?
 This leads us to the question of whether or not coblation is better than other surgical methods such as electrocautery. When this technology was initially released it was touted as a better way to perform a tonsillectomy because the low heat did not destroy healthy tissue. It’s said that as a result of using low heat, the patient experiences less pain and bleeding after the operation. Ask anyone who has experienced tonsillectomy and they will tell you that the recovery period is not at all pleasant.
This leads us to the question of whether or not coblation is better than other surgical methods such as electrocautery. When this technology was initially released it was touted as a better way to perform a tonsillectomy because the low heat did not destroy healthy tissue. It’s said that as a result of using low heat, the patient experiences less pain and bleeding after the operation. Ask anyone who has experienced tonsillectomy and they will tell you that the recovery period is not at all pleasant.
While many physicians believe that coblation is a safer, gentler method, a recent paper “Coblation versus other surgical techniques for tonsillectomy” suggests that there is little-supporting evidence showing this method to be superior. The paper examined 29 previous studies, concluding that there was not much evidence to support that the claims of coblation being a less painful procedure are true.
Dr. Melissa Ann Pynnonen, a professor in Michigan Medicine’s Department of Otolaryngology, believes that the marketing efforts by medical device companies have caused people to believe that coblation makes the procedure less painful.
In other words, regardless of the method used to remove your tonsils, swallowing is going to be painful for at least 14 days.
Alternative to Tonsillectomy
 Maybe you are thinking to yourself that a tonsillectomy doesn’t sound like something you would like to experience. Is there an alternative to having a Tonsillectomy? Actually, there is.
Maybe you are thinking to yourself that a tonsillectomy doesn’t sound like something you would like to experience. Is there an alternative to having a Tonsillectomy? Actually, there is.
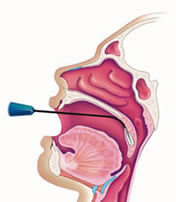
In the early 2000’s a new procedure was approved by the Food and Drug Administration (FDA). Rather than removing your tonsils, Somnoplasty allows you to keep your tonsils in place while reducing their size. While this procedure can be helpful to those who experience snoring or sleep apnea, patients who experience frequent infections in their tonsils typically will not benefit.
The procedure involves inserting electrodes into the tonsils and delivering RF energy directly within the tonsils. These electrodes are very thin and needle-like. The needle/ electrode is insulated with the exception of the tip. The energy delivered selectively destroys tissue and causes the tonsils to shrink from within. While the tonsils will still be present, they will become much smaller which can prevent them from interfering with breathing and causing snoring or sleep apnea.
This is typically an outpatient surgery that is performed under local anesthesia. The procedure typically takes between 30-45 minutes from start to finish.
The benefit of having a Somnoplasty instead of Tonsillectomy is less pain and post-operation bleeding.
If you are suffering from snoring or sleep apnea and are considering a tonsillectomy, you may want to speak with your doctor about having a somnoplasty instead.
Share This Post:
 According to the manufacturer, the SnoreCare nose cones are made from a high quality, soft medical grade silicone that is BPA free.
According to the manufacturer, the SnoreCare nose cones are made from a high quality, soft medical grade silicone that is BPA free. The claim that SnoreCare makes is quite simple – it will stop your snoring, but the question is how does it stop snoring? They do offer an explanation.
The claim that SnoreCare makes is quite simple – it will stop your snoring, but the question is how does it stop snoring? They do offer an explanation. The SnoreCare website has their product listed at $16.95 plus the cost of shipping and taxes. When I tried to place an order I was unable to do so because the checkout was disabled.
The SnoreCare website has their product listed at $16.95 plus the cost of shipping and taxes. When I tried to place an order I was unable to do so because the checkout was disabled. The SnoreCare nose vents arrived as a set of four as promised along with a travel case. The SnoreCare was made from a soft silicone-like material and seemed to be of good quality.
The SnoreCare nose vents arrived as a set of four as promised along with a travel case. The SnoreCare was made from a soft silicone-like material and seemed to be of good quality. Oversleeping, long sleeping, sleeping too much, hypersomnia – no matter what you call it, we are referring to the same condition. It comes down to knowing whether you are getting too much or too little sleep every night.
Oversleeping, long sleeping, sleeping too much, hypersomnia – no matter what you call it, we are referring to the same condition. It comes down to knowing whether you are getting too much or too little sleep every night. There are several questions that you should ask yourself when investigating your sleeping habits. Do you consume an excessive amount of alcohol before going to bed? Do you take sedatives, prescription medication, or other drugs that may disrupt your sleep and cause you to stay in the bed longer? What about caffeinated beverages before bed? All of these items may cause you to sleep in excess.
There are several questions that you should ask yourself when investigating your sleeping habits. Do you consume an excessive amount of alcohol before going to bed? Do you take sedatives, prescription medication, or other drugs that may disrupt your sleep and cause you to stay in the bed longer? What about caffeinated beverages before bed? All of these items may cause you to sleep in excess. How do you feel upon rising after getting 9+ hours of sleep? Do you feel refreshed and ready to conquer the day or do you still feel tired, sluggish and could continue to sleep? If you still feel tired even after getting more than the recommended amount of sleep, this may be caused by a sleep disorder or breathing-related sleep disorder such as
How do you feel upon rising after getting 9+ hours of sleep? Do you feel refreshed and ready to conquer the day or do you still feel tired, sluggish and could continue to sleep? If you still feel tired even after getting more than the recommended amount of sleep, this may be caused by a sleep disorder or breathing-related sleep disorder such as  When a person discovers that they snore, the first question that they are likely to ask is whether or not snoring is normal.
When a person discovers that they snore, the first question that they are likely to ask is whether or not snoring is normal. When snoring becomes abnormal, you do have several options to correct the issue.
When snoring becomes abnormal, you do have several options to correct the issue.
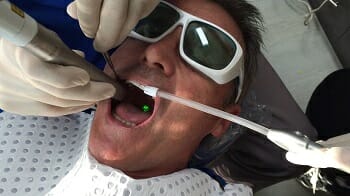
 With an 80% success rate, NightLase seems to be one of the more effective snoring solutions available. Being non-invasive and not causing any permanent changes in the structure of the airway are two desirable features of this procedure compared to surgeries that are permanent and can cause complications later down the road. With the NightLase, you will not be dependent on the nightly use of oral appliances.
With an 80% success rate, NightLase seems to be one of the more effective snoring solutions available. Being non-invasive and not causing any permanent changes in the structure of the airway are two desirable features of this procedure compared to surgeries that are permanent and can cause complications later down the road. With the NightLase, you will not be dependent on the nightly use of oral appliances.


 There are two different types of mouthpieces that are available – MAD’s and TSD’s. Here are a couple quick tests that you can try at home to help determine if either product will work for you.
There are two different types of mouthpieces that are available – MAD’s and TSD’s. Here are a couple quick tests that you can try at home to help determine if either product will work for you. You’re probably wondering if the snoring mouthpiece is 100% effective. While I have had great success using one myself as well as several close friends and family members that I recommended them to, a mouthpiece may not be the solution for everyone. While effectiveness seems to vary from one study to another, they seem to be effective somewhere between 80% and 90% of cases, which is higher than any other snoring solution out there. In fact, no other anti-snoring product has been studied nearly as much as the snoring mouthpiece. Physicians have known about their effectiveness since the 1980’s.
You’re probably wondering if the snoring mouthpiece is 100% effective. While I have had great success using one myself as well as several close friends and family members that I recommended them to, a mouthpiece may not be the solution for everyone. While effectiveness seems to vary from one study to another, they seem to be effective somewhere between 80% and 90% of cases, which is higher than any other snoring solution out there. In fact, no other anti-snoring product has been studied nearly as much as the snoring mouthpiece. Physicians have known about their effectiveness since the 1980’s. While learning about snoring mouthpieces, you have probably seen advertisements stating that a product is “FDA approved” or “FDA cleared”. Technically speaking, the FDA doesn’t necessarily approve any mouthpieces. While this term is often used loosely by advertisers, “FDA Approved” wording is actually prohibited from being used all together. Most sellers unknowingly use this term in lieu of the correct term which is actually FDA cleared.
While learning about snoring mouthpieces, you have probably seen advertisements stating that a product is “FDA approved” or “FDA cleared”. Technically speaking, the FDA doesn’t necessarily approve any mouthpieces. While this term is often used loosely by advertisers, “FDA Approved” wording is actually prohibited from being used all together. Most sellers unknowingly use this term in lieu of the correct term which is actually FDA cleared. When shopping for a mouthpiece, you see if the words “FDA Cleared” are written within an ad. Do you stop there and take their word for it? Probably not. Before making a decision it’s a good idea to search the
When shopping for a mouthpiece, you see if the words “FDA Cleared” are written within an ad. Do you stop there and take their word for it? Probably not. Before making a decision it’s a good idea to search the 


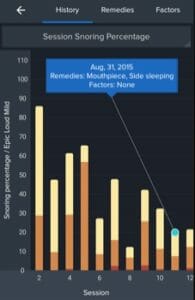
 Snore Clock by Ralph Schiffhauer is another popular snoring app that was awarded app of the month by MIT technology. The features of this product are similar to that of SnoreLab, although Snore Clock does not assign a snore score.
Snore Clock by Ralph Schiffhauer is another popular snoring app that was awarded app of the month by MIT technology. The features of this product are similar to that of SnoreLab, although Snore Clock does not assign a snore score. Do I Snore or Grind (yes, that’s the name of the app) by Sleep.ai.B.V. combines the ability to detect both teeth grinding and snoring. This app allows you to choose your desired mode – snoring, grinding or both. When activated, it listens throughout the night and uses an algorithm to determine whether the sounds coming from your bedroom are snoring or teeth grinding while filtering all other sound.
Do I Snore or Grind (yes, that’s the name of the app) by Sleep.ai.B.V. combines the ability to detect both teeth grinding and snoring. This app allows you to choose your desired mode – snoring, grinding or both. When activated, it listens throughout the night and uses an algorithm to determine whether the sounds coming from your bedroom are snoring or teeth grinding while filtering all other sound.